A Methodology for Activity-Based Costing to Scale IVF Lab Operations
Conceivable Life Sciences, 2025
Table Of ContentsIntroduction
Economic Cost Breakdown
Conclusions
Looking Forward
Synopsis
Background The fertility services market exceeds $25 billion annually, yet cost analysis of in vitro fertilization (IVF) operations remains limited. Traditional cost accounting fails to capture the complex relationship between biological and disposable inputs, skilled labor, and specialized equipment utilization.
Objective To develop a microeconomic framework to improve decision-making by properly measuring cost structures and scale economies in fertility services using activity-based costing (ABC) methodology.
Methods We analyzed data from five IVF laboratories (600-2,200 annual cycles) across different U.S. regions, conducting time studies of 500+ procedures. We developed econometric models to quantify cost elasticity and scale effects.
Results IVF procedures demonstrate significant cost elasticity relative to biological inputs: egg freezing, standard IVF, and IVF with biopsy. We identified substantial scale economies, with marginal costs 40% higher in 500-cycle labs versus 2000-cycle labs, and 13% lower in 4000-cycle labs. Labor efficiency increases by 30% between 500-cycle and 2000-cycle operations, while capital utilization improves dramatically. Current flat-rate pricing creates allocative inefficiencies, with price-to-marginal-cost ratios varying significantly across biological input levels and lab scale.
Conclusions The significant cost elasticity and scale economies documented in this paper provide economic rationale for IVF lab (capacity) consolidation and suggest welfare-enhancing alternatives to current pricing models. Our methodology offers a template for analyzing other specialized healthcare services combining variable biological inputs, specialized capital, and skilled labor.
KEY WORDSHealthcare economics • Cost elasticity • Scale economies • Fertility services • Activity-based costing
Prologue: The IVF Inflection Point
Infertility is a continuous epidemic touching the lives of 1 in 6 people globally—17% of the population struggling with one of humanity's most fundamental desires: to create a family. Despite affecting millions, infertility treatment remains largely a privilege rather than a right, with In Vitro Fertilization (IVF) established as expensive concierge medicine available primarily to the wealthy or fortunate few with comprehensive insurance coverage.
The contemporary IVF laboratory is a study in contrasts: scientifically advanced yet operationally antiquated. These highly manual environments operate with tremendous variability—from unstandardized protocols and inconsistent outcomes to widely differing cost structures. This variability manifests not just in success rates but in resource utilization, staffing models, and ultimately, in the financial burden placed on patients. A single IVF cycle can range from $12,000 to $30,000, with many patients requiring multiple attempts, placing this essential medical treatment beyond the reach of most Americans. In fact, we estimate that based on current birth rates combined with infertility and miscarriage rates by age group, there are at least 550,000 women/ couples in the US attempting to have a baby each year but can not due to infertility factors. Unfortunately, only 175,000 of them can afford to start an IVF retrieval or donor cycle, or less than 33%. If clinics can find innovative ways to significantly reduce costs and fees, they can scale to target and bring hope to the unserved 67%.
Automation represents a paradigm shift in addressing these challenges. Automated IVF laboratories can standardize protocols, reduce human error, optimize resource utilization, and dramatically increase throughput while maintaining or improving quality. The precision of robotics combined with the analytical power of artificial intelligence creates both consistency and efficiency—the foundations of both improved clinical outcomes and economic accessibility.
Activity-based costing (ABC) offers a powerful methodology to address these challenges. Over more than a decade of speaking to senior IVF operators, we have found wildly different approaches to analyzing costs associated with running their labs.
As innovation in the IVF sector accelerates, it struck us as a valuable exercise to develop a universal approach to establishing clarity and an accurate accounting of costs.
So what is activity-based costing? It is a methodology that identifies activities within an enterprise and assigns the cost of each activity to products or services according to their actual consumption, providing a more accurate determination of true costs than traditional costing methods.
While not the most romantic lens through which to view laboratories dedicated to creating life, fertility clinics are, at their core, sophisticated artisan manufacturing environments. They represent specialized production systems that transform unique inputs through precisely controlled processes, utilizing highly specialized labor, advanced equipment, and meticulously regulated environmental conditions.
Yes, our inputs are the profound biological materials of sperm and egg, and our outputs are embryos that may become not just babies but the fulfillment of deeply personal dreams. However, reframing these laboratories through the clinical precision of operational management reveals transformative insights that will lead to greater efficiency, quality, and ultimately, success rates.
This operational perspective doesn't diminish the miracle—it enhances our ability to consistently create it.
In our research we found a number of surprising, sometimes counterintuitive results. For example, the number of eggs collected matters: a low stimulation approach can significantly improve profitability, while high egg production makes costs soar dramatically due to increased labor costs.
Developing a methodology and a benchmarking system to compare costs as apples to apples means we can create an industry standard for operators to truly understand costs of operations. This framework allows for detailed analysis that dissects all operational costs— from procedure volumes and staff compensation to supplies, capital equipment, facilities overhead, and administrative expenses—creating transparency across clinical enterprises regardless of their size or ownership structure.
The convergence of automation technology and activity-based costing methodology creates a powerful force for democratizing fertility care. By precisely understanding true costs and leveraging the efficiencies of automation, we can reimagine the economics of IVF. This isn't merely an academic exercise—it is the foundation for a future where reproductive technology is accessible to all who need it, with higher success rates, fewer treatment cycles, and substantially lower patient costs. The miracle of life creation need not be reserved for the privileged few; through operational excellence and economic transparency, we can extend this profound opportunity to the millions who deserve it.
Introduction
In vitro fertilization (IVF) has evolved from an experimental procedure to a standardized treatment that has helped millions of people build families. Despite its growing prevalence, the economics of IVF operations remain opaque, with costs varying dramatically across regions and clinics. This lack of transparency hinders market efficiency, disadvantages patients, and impedes the scaling of fertility treatments to meet growing global demand.
The fertility sector is experiencing unprecedented investment and consolidation, yet it lacks the sophisticated cost analysis frameworks common in other healthcare segments. Most IVF clinics still rely on simplistic accounting methods that fail to capture the true economics of their complex operations. Activity-based costing (ABC) provides a solution, offering a methodology that can transform how fertility clinics understand and improve their operations, set prices, and scale their services.
Reframing IVF Labs as ‘Specialized Manufacturing Operations’ A typical IVF laboratory functions essentially as an artisan manufacturing shop—a specialized production environment that creates outputs through the complex conversion of inputs using specialized labor, equipment, and controlled environmental conditions. This reframing has profound implications for operational management.
Traditional accounting in IVF clinics often assigns labor, supplies, overhead, and capital costs using simplistic measures like total procedure counts. This creates a distorted view of profitability across different procedures and patient characteristics. If every IVF cycle is assigned the same average labor and overhead regardless of complexity, clinics cannot accurately determine where profits come from or how to optimize their operations.
Activity-based costing traces costs to the specific activities that consume resources to convert inputs into desired outputs. This approach reveals the true economics of different procedures and patient characteristics and needs, providing a foundation for strategic decision-making.
The ABC Methodology Applied to IVF The implementation of ABC analysis for IVF operations follows a structured methodology:
Activity Mapping: Identify and document all activities performed to convert inputs in each procedure's value stream, from initial consultation through to retrieval, fertilization, embryo development, biopsy and then to transfer or cryopreservation.
Time Determination: Calculate both fixed time components (setup, witnessing, cleanup, documentation) and variable time components (per egg or embryo) required by each staff role and equipment type to perform each activity.
Direct Cost Calculation: Compute direct costs (labor = time × fully-burdened rate, plus supplies) for each activity, incorporating all employee costs including recruitment, training, and professional development.
Indirect Cost Allocation: Distribute indirect costs (overhead, rent, utilities, gases, liquid nitrogen) and fixed costs (equipment and facility capital charges) based on the relative usage of personnel, equipment, and floor space across different value streams.
Quality Cost Assessment: Determine the cost of quality, or rework costs, based on procedure-specific error rates that lead to patient compensation with replacement cycles.
Operational Variability Analysis: Calculate how true economic costs vary under different operational scenarios—such as staff compensation levels, eggs retrieved, procedure mix, lab scale, and procurement discounts.
Once implemented, this methodology provides a multidimensional cost model that reveals insights impossible to obtain through traditional accounting. It demonstrates how costs vary not just between procedures, but within procedures based on biological factors like egg or embryo count and operational factors like lab scale.
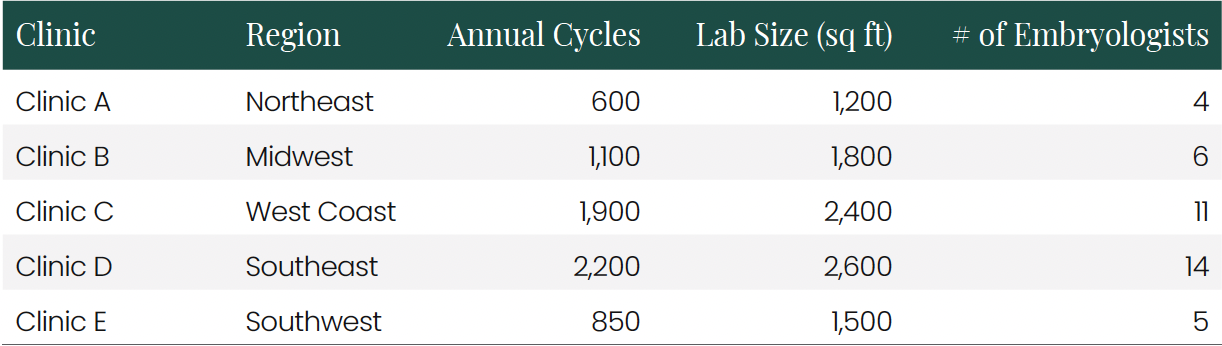
Multi-Clinic Data Analysis The analysis presented here synthesizes data from five anonymous IVF clinics across different regions, representing a range of operational scales:
This diverse dataset allows for the identification of cost patterns that transcend regional variations and reveals how scale affects operational economics. The clinics vary not only in size but also in their procedure mix, with some focusing more heavily on egg freezing while others emphasize genetic testing or donor services.
The data synthesis methodology employed a standardized activity mapping approach to ensure comparability across clinics despite differences in protocols and terminology. Time studies were conducted at each location, with over 500 procedures observed across all five clinics to establish reliable time standards for each activity.
Revealing Cost Structures and Variations Using ABC analysis, we can see that IVF lab costs vary across multiple dimensions that traditional accounting methods miss entirely. The accompanying figures illustrate two key findings from an analysis of different IVF procedures at different biological input levels and at different lab scales.
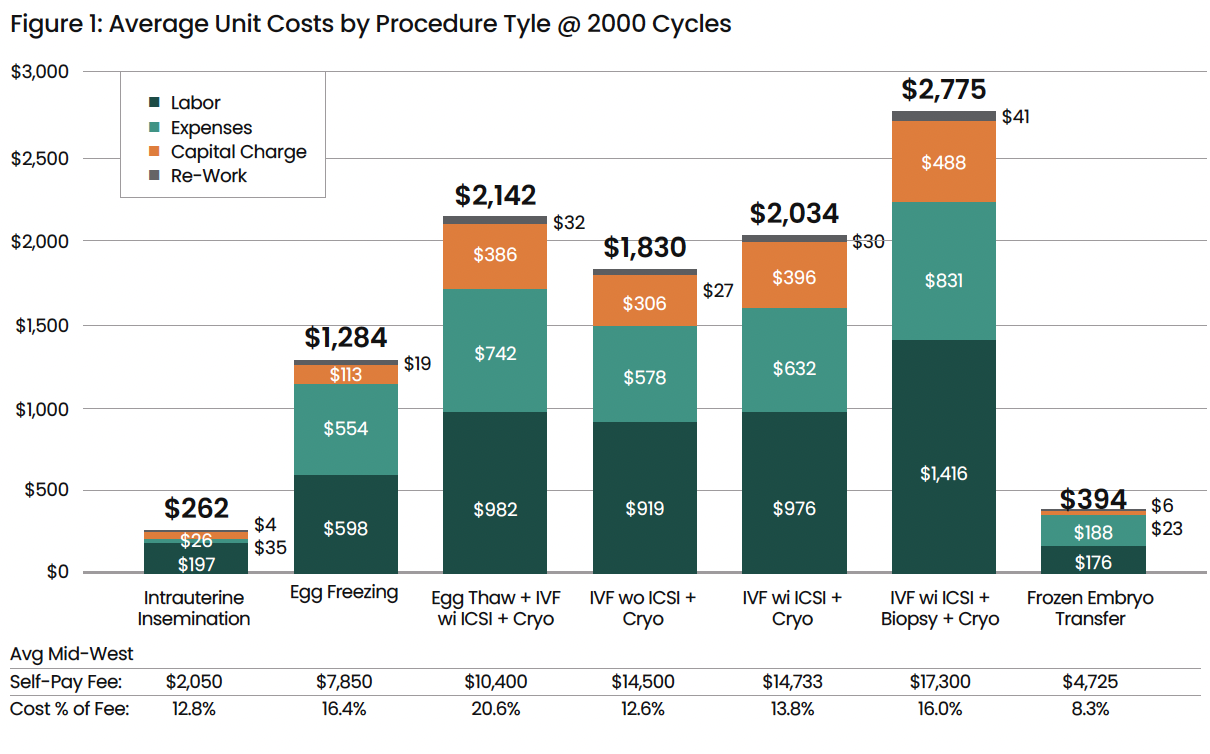
Figure 1 reveals the dramatic variation in procedure costs across different types of IVF services. While simplistic accounting might calculate an average labor cost of approximately $1,126 for egg-based procedures, the ABC analysis shows actual costs ranging from $598 to $1,416 depending on the specific procedure. Similarly, when indirect expenses are fully allocated, unit expenses average $686 but vary considerably by procedure type. Capital charges, often overlooked in operational decisions, average $465 per procedure but show significant procedure-dependent variation based on relative usage of equipment.
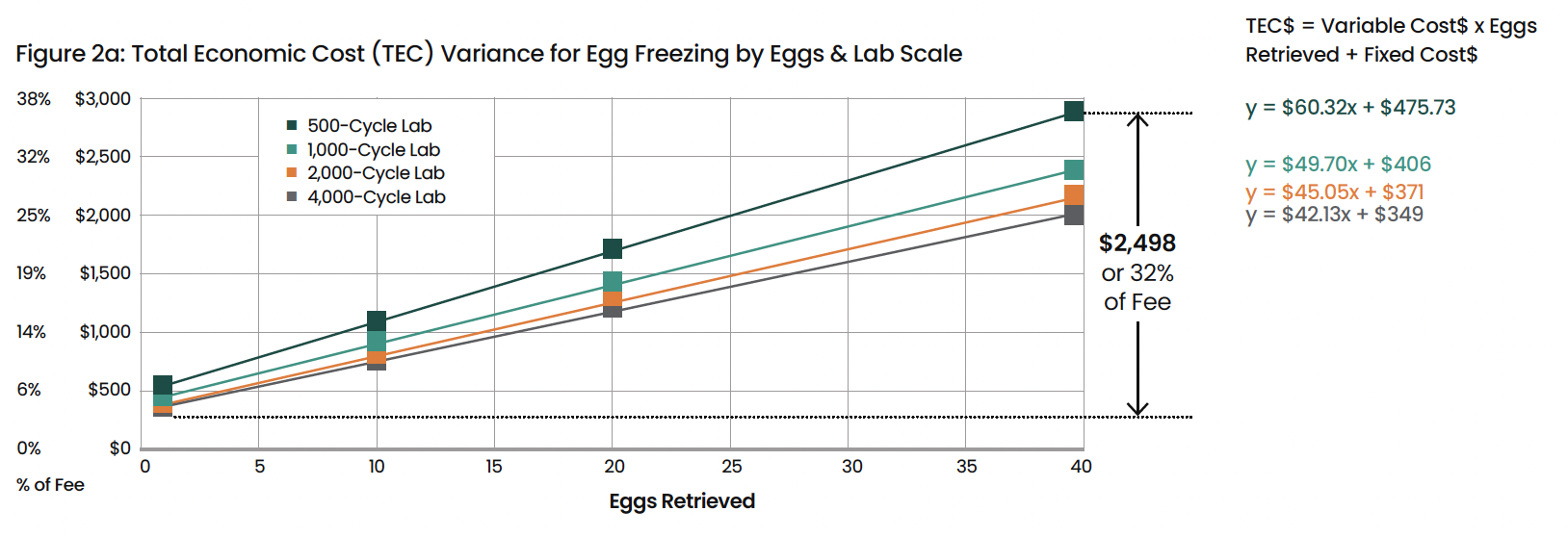
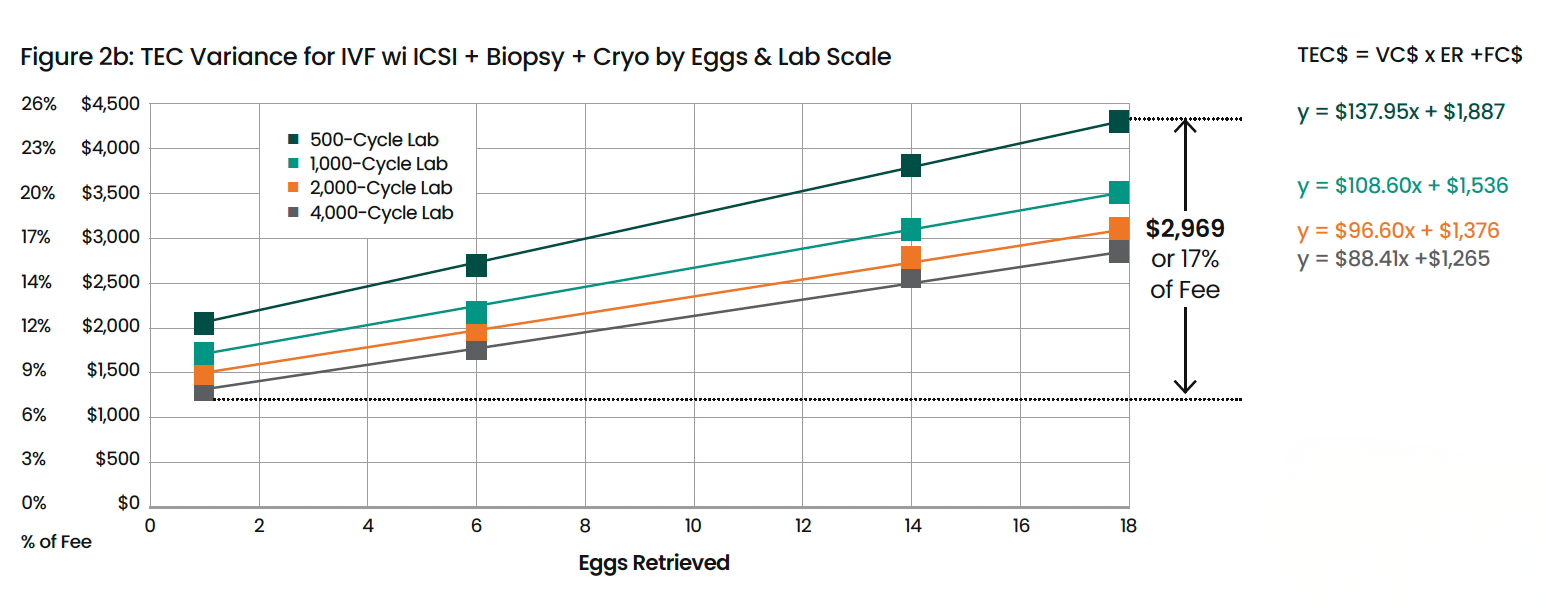
But even more revealing is how costs vary dramatically within the same procedure based on biological factors and lab scale. Figure 2 illustrates how procedure costs increase with egg count and decrease with lab scale, demonstrating the concept of "cost elasticity" (CE)—the percentage change in cost relative to the percentage change in input volume.
Figures 2a,b: Cost Variation by Egg Count and Lab Scale
The detailed activity-based cost model for IVF laboratory operations enables detailed analysis across all key dimensions:
Procedures (and supporting activities)
Productivity
Regional and role-based labor rates
Burden rate (turnover, payroll taxes, benefits, savings, prof development)
Supplies used and purchasing discount
Error rates
Equipment used
Rent
Egg/ embryo volume per procedure
Patient/ lab volume
For egg freezing, the analysis reveals that costs increase by 165% when egg volume increases by 300%, giving a cost elasticity of 55%. This means that procedures with higher egg counts appear disproportionately more expensive than suggested by the raw egg count. For IVF with ICSI, biopsy, and cryopreservation, costs increase by 59% when egg volume increases by 200%, giving a cost elasticity of 30%.
The figures also demonstrate the significant impact of scale. A 4000-cycle lab achieves 24-30% lower cost per procedure compared to a 500-cycle lab, underscoring the economic rationale for lab centralization and consolidation in the fertility industry.
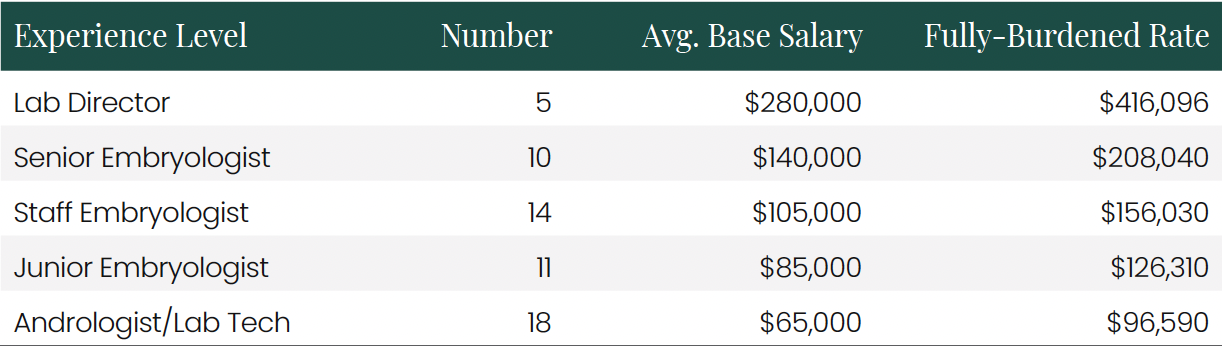
Staffing Structure and Embryologist Economics A critical component of IVF lab costs is personnel, particularly embryologists. The analyzed clinics employed a total of 40 embryologists with varying experience levels:
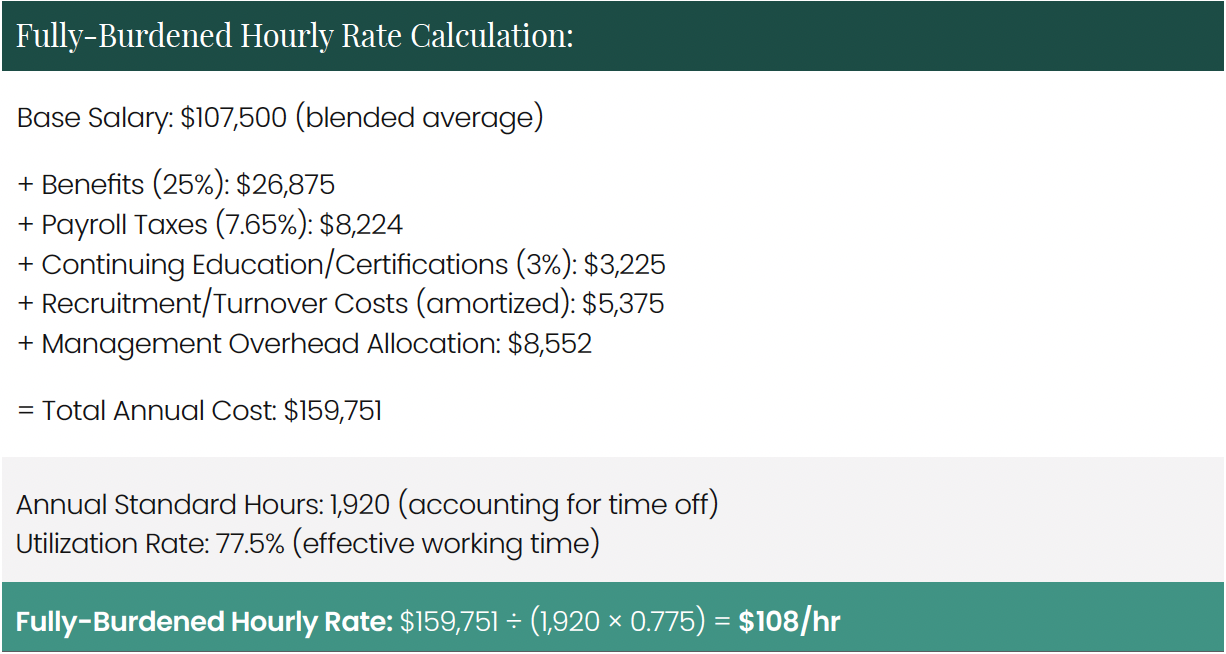
The fully-burdened hourly cost calculation for embryologists reveals the true cost of these highly specialized professionals:
With lab protocols requiring dual witnessing for critical steps, the effective hourly rate often increases further as two embryologists are simultaneously engaged in a single procedure.
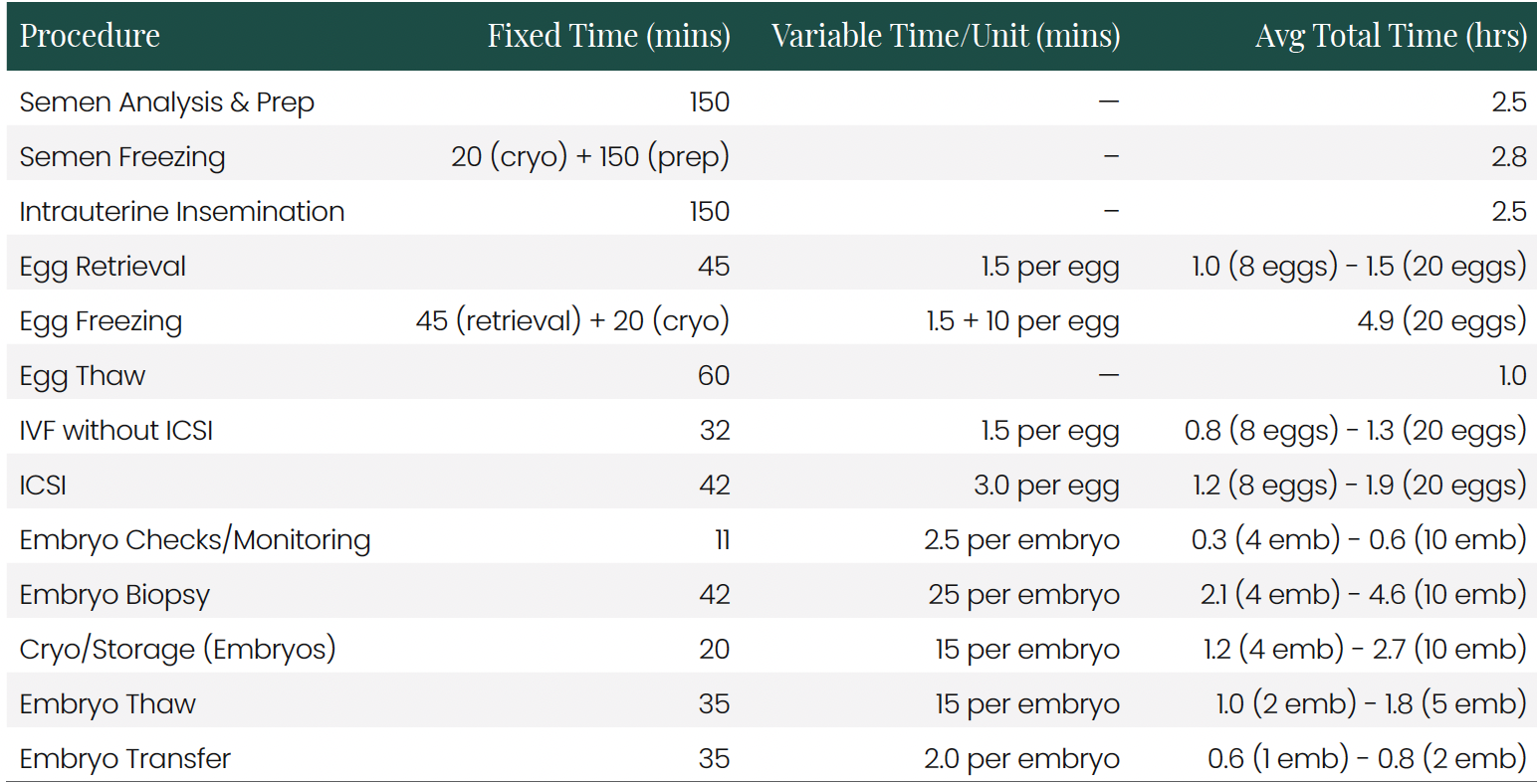
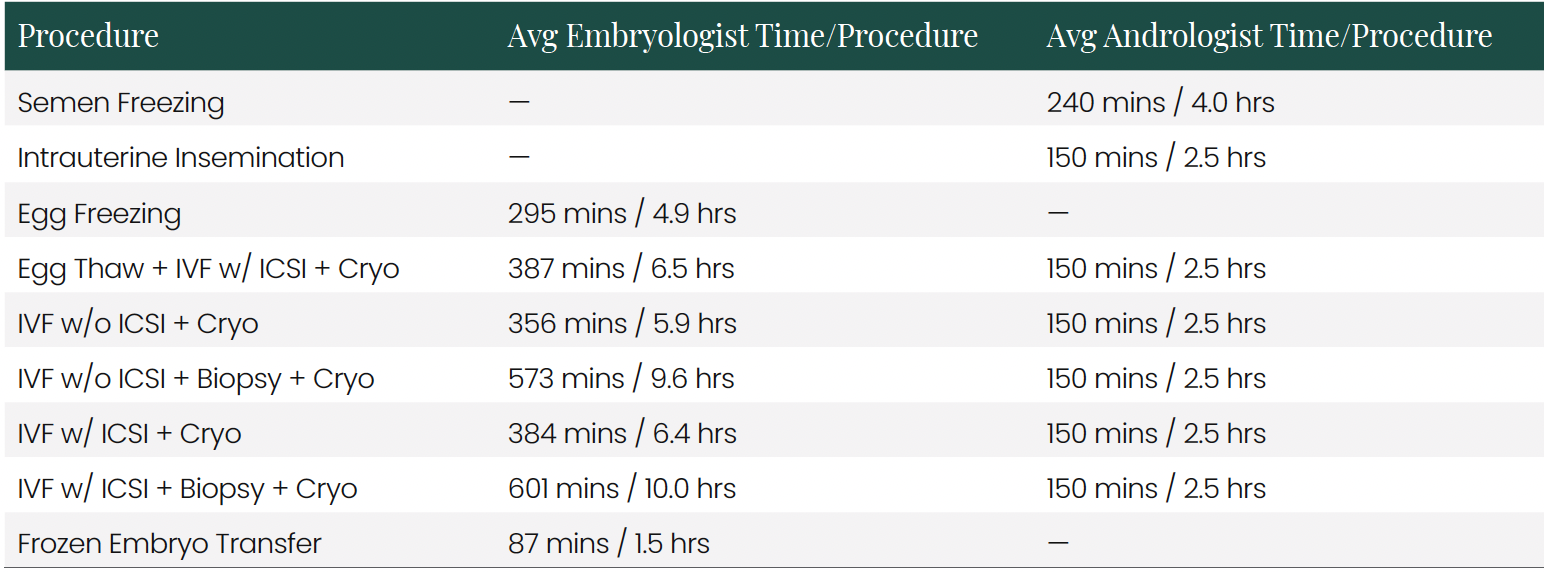
Time Standards by Procedure The time study results revealed significant variations in time requirements across procedures:
These time standards demonstrate the critical difference between fixed and variable time components. Fixed time includes setup, documentation, and cleanup activities that remain relatively constant regardless of egg/embryo count. Variable time scales with biological volume, creating the cost elasticity observed in the analysis.
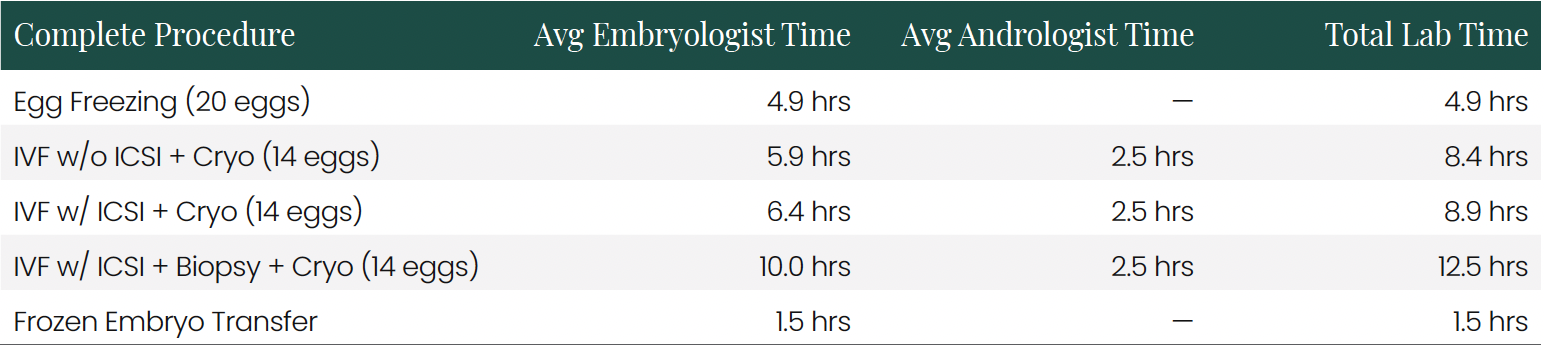
When aggregated into complete procedure paths, the time requirements become more substantial:
The substantial time requirements for complex procedures like IVF with ICSI, biopsy, and cryopreservation explain their high costs. At fully-burdened rates of $108/hour for embryologists and $66/hour for andrologists, direct labor costs alone for these procedures range from $531 (Egg Freezing) to $1,248 (IVF with ICSI, Biopsy, and Cryopreservation).
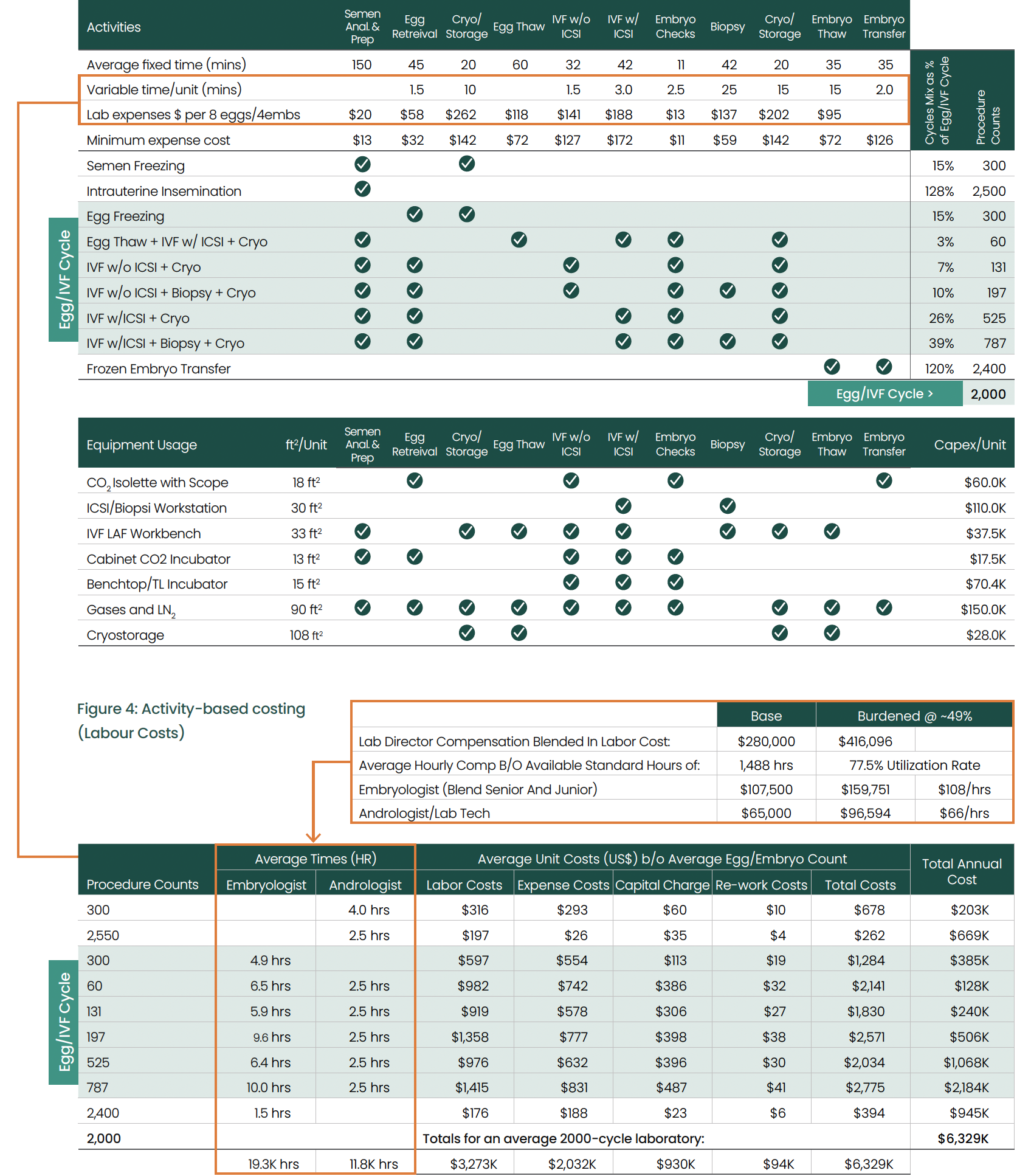
The Economics of a 2000-Cycle Lab
1. Procedure Distribution
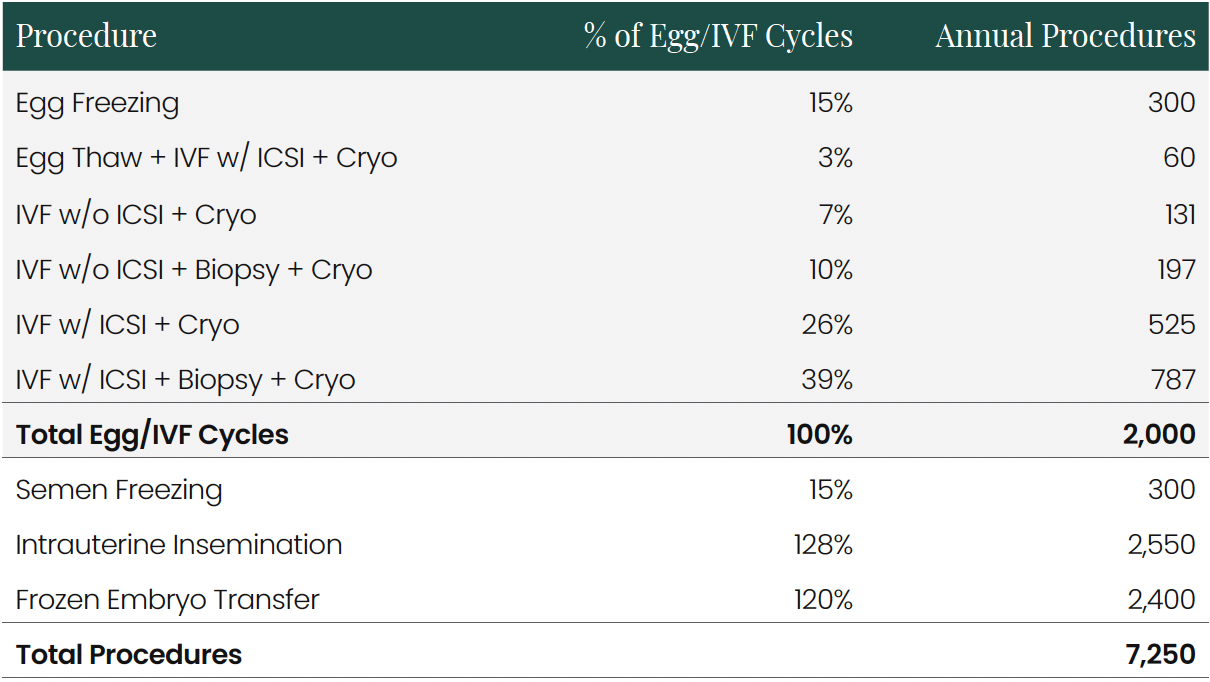
A nominal 2000-cycle IVF laboratory in the Midwest US offers a range of fertility services with the following procedure distribution:
Note: The percentages for semen freezing, IUI and FET represent the ratio of these procedures to the base 2000 egg/IVF cycles.
2. Labor
2.1 Labor Time By Procedure
Total annual standard hours: 19,251 embryologist hours and 11,825 andrologist hours
This translates to staffing requirements of approximately 12.9 embryologists and 7.9 andrologists.
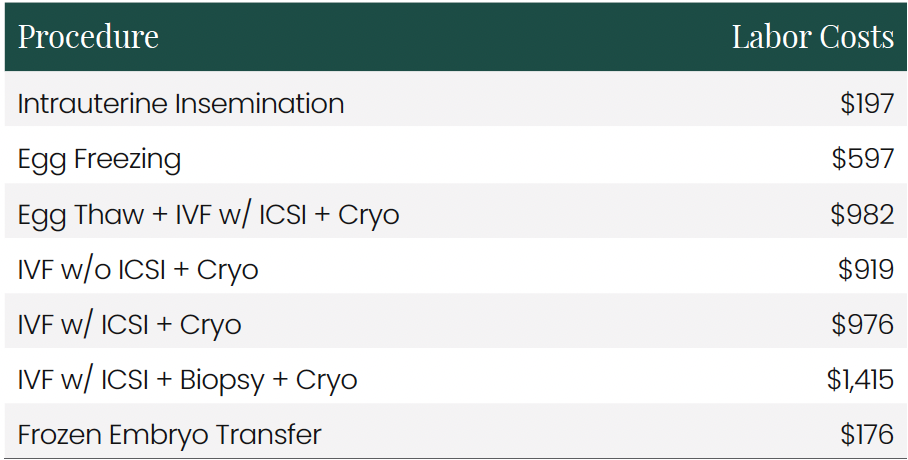
2.1 Labor Cost By Procedure
Labor cost calculation (table 2.1 and figure 4) based on:
Embryologist (blend of Senior and Junior): $107,500 base ▶ $159,751 fully-burdened ▶ $108/hr
Andrologist/Lab Tech: $65,000 base ▶ $96,594 fully-burdened ▶ $66/hr
Lab Director: $280,000 base ▶ $416,096 fully-burdened ÷ 31,076 lab staff hours ▶ $13/hr
Total annual labor costs: $3,273,000
3. Supplies
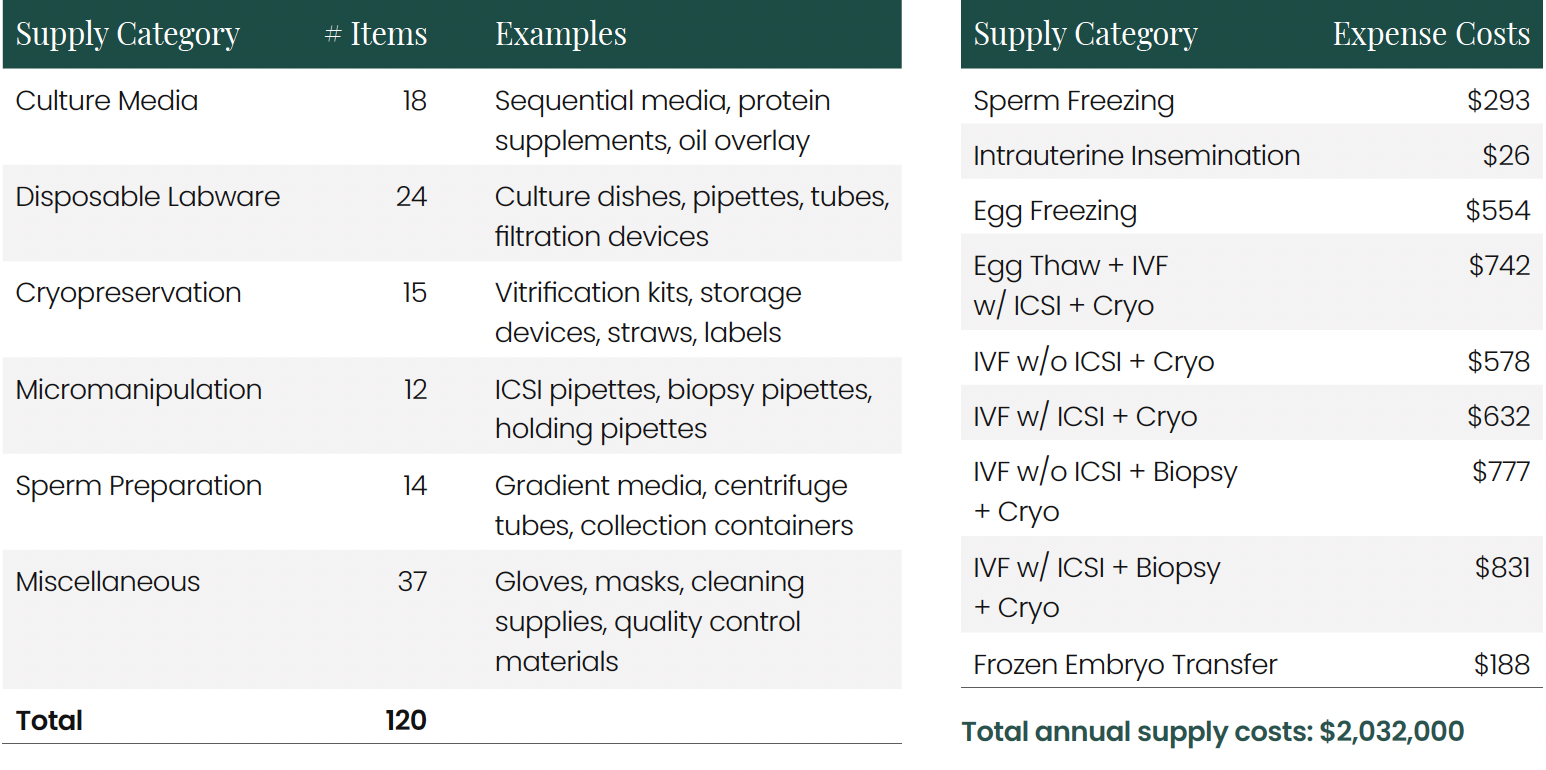
3.1 Supplies Used Across Procedures
3.2 Supplies Cost By Procedure
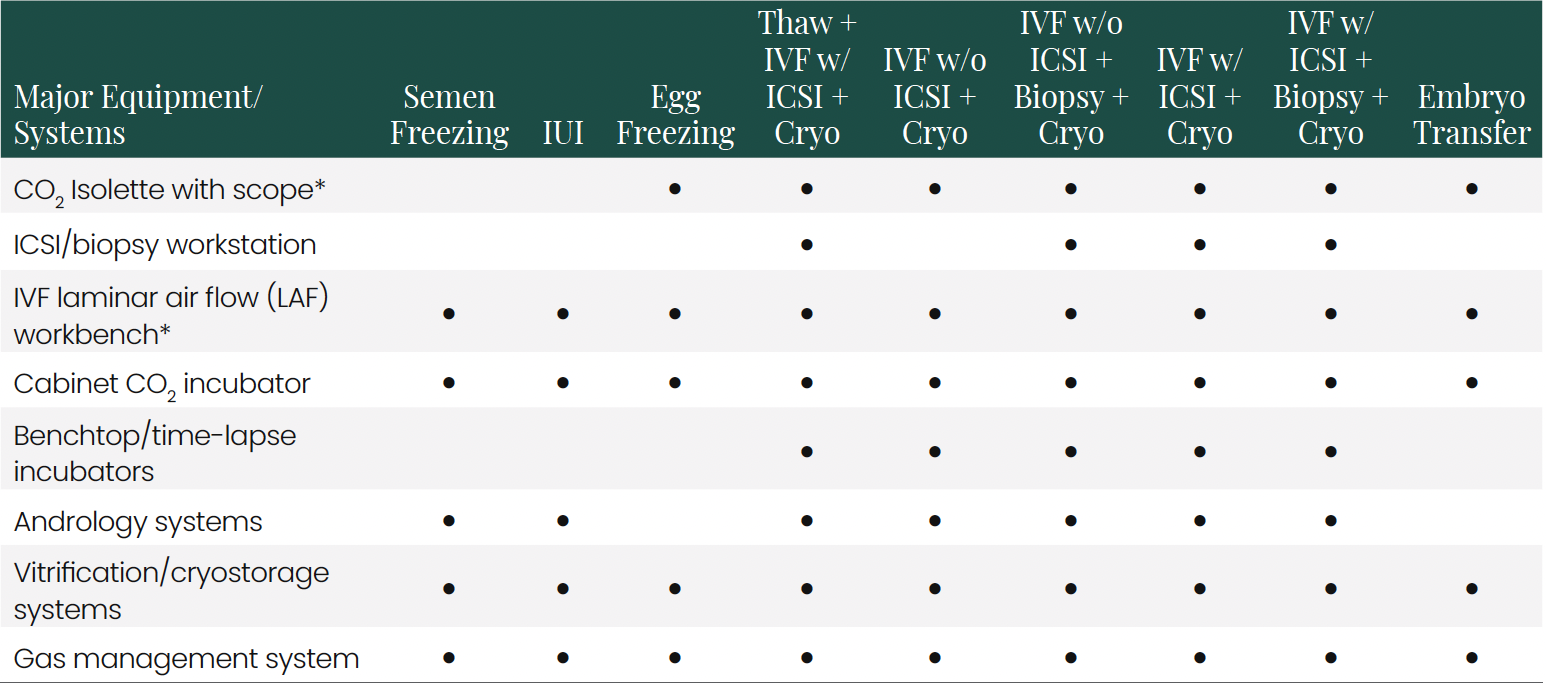
4. Equipment and Space
4.1 Equipment Use By Procedure
*Note: Some labs only use IVF LAF workbenches instead of CO2 Isolettes based on Air Handling Unit (AHU) and media
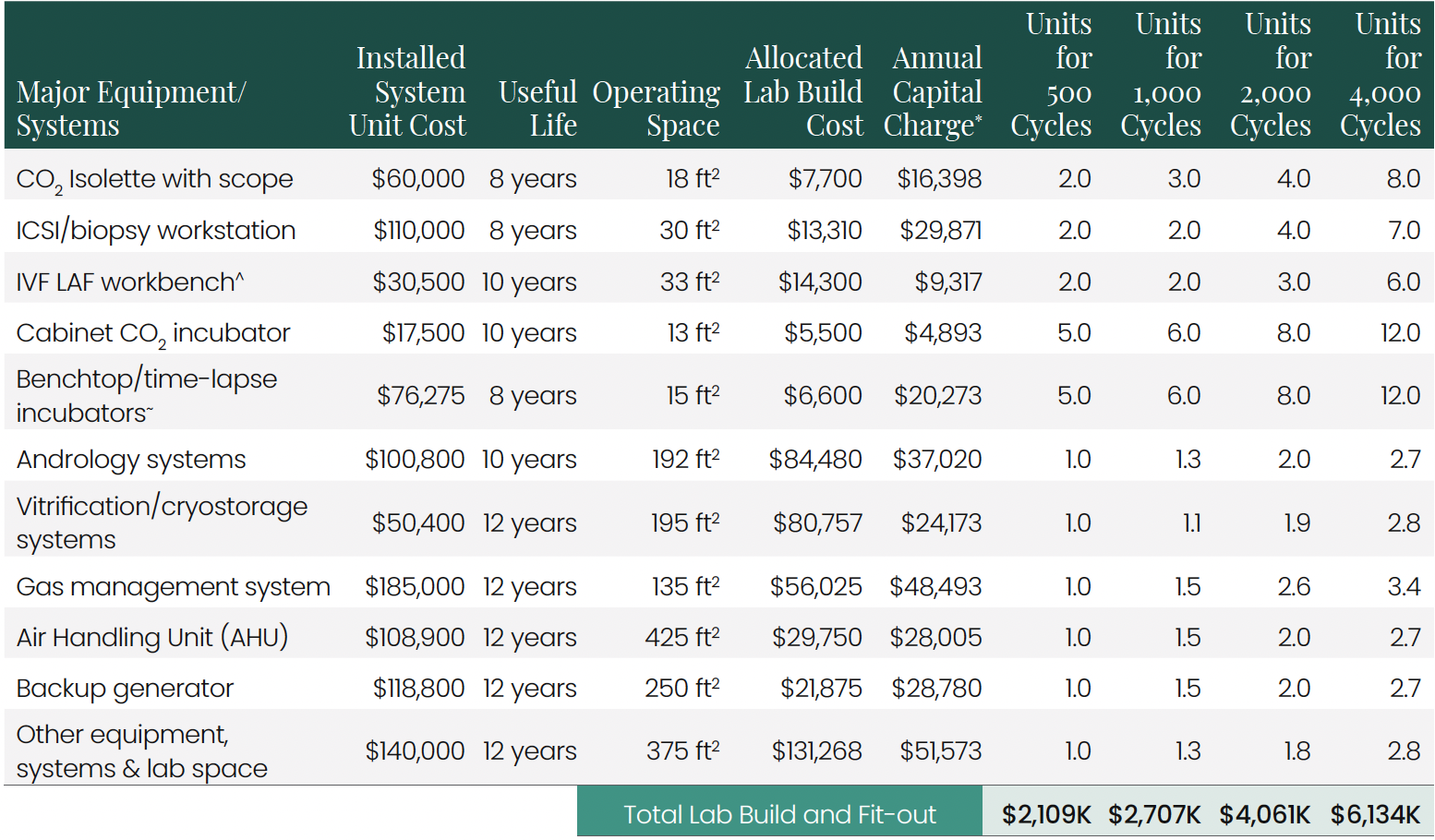
4.2 Equipment Installed Cost and Required Space By Lab Scale
*Annual capital charge includes maintenance, calibration, and WACC charge of 12% for equipment AND space build cost
^ Blend of IVF LAF workbenches with and without scopes and heated plates
~ Blended average of benchtop and time-lapse incubators
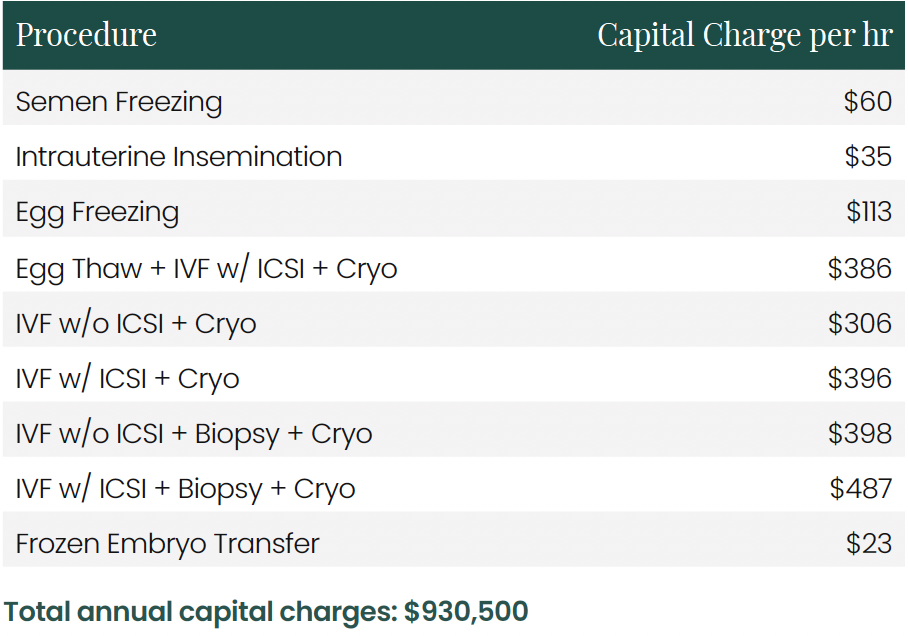
4.3 Capital Charge by Procedure
5. Total
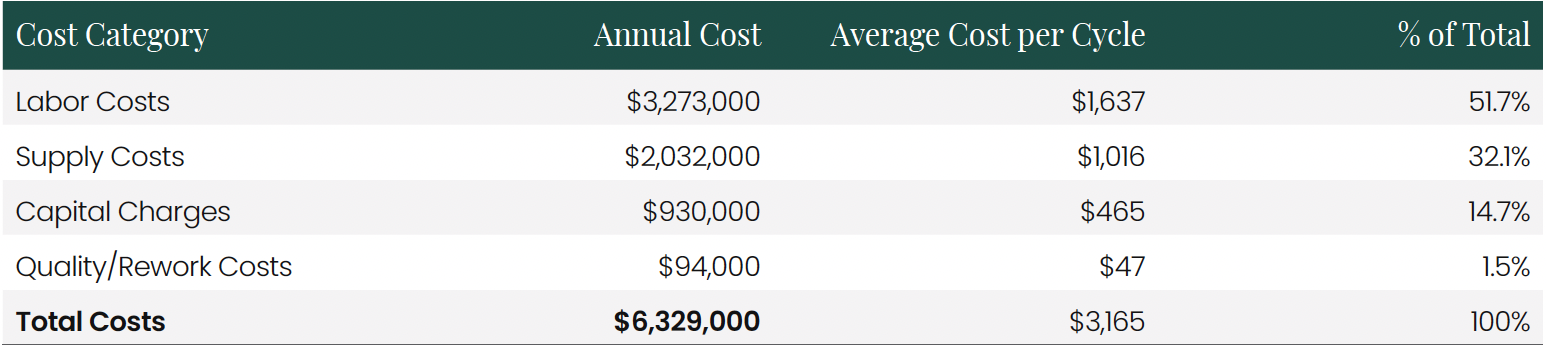
5.1 Annual Operating Expenses (2000-Cycle Lab)
The average total unit cost by procedure:
Intrauterine Insemination: $262
Egg Freezing: $1,284
Egg Thaw + IVF w/ ICSI + Cryo: $2,142
IVF w/o ICSI + Cryo: $1,830
IVF w/ ICSI + Cryo: $2,034
IVF w/ ICSI + Biopsy + Cryo: $2,775
Frozen Embryo Transfer: $394
Total annual operating expenses for a 2000-cycle IVF lab in the Midwest US: $6,329,000
Lab space required: 2,400 ft² with average rent cost of $48/ft²
Note: The following data is based on a conservative synthesis of activity, supplies and equipment data from 4 IVF labs.
Figure 3: Activity-based costing for a 2000-cycle lab (Procedures and Equipment Usage)
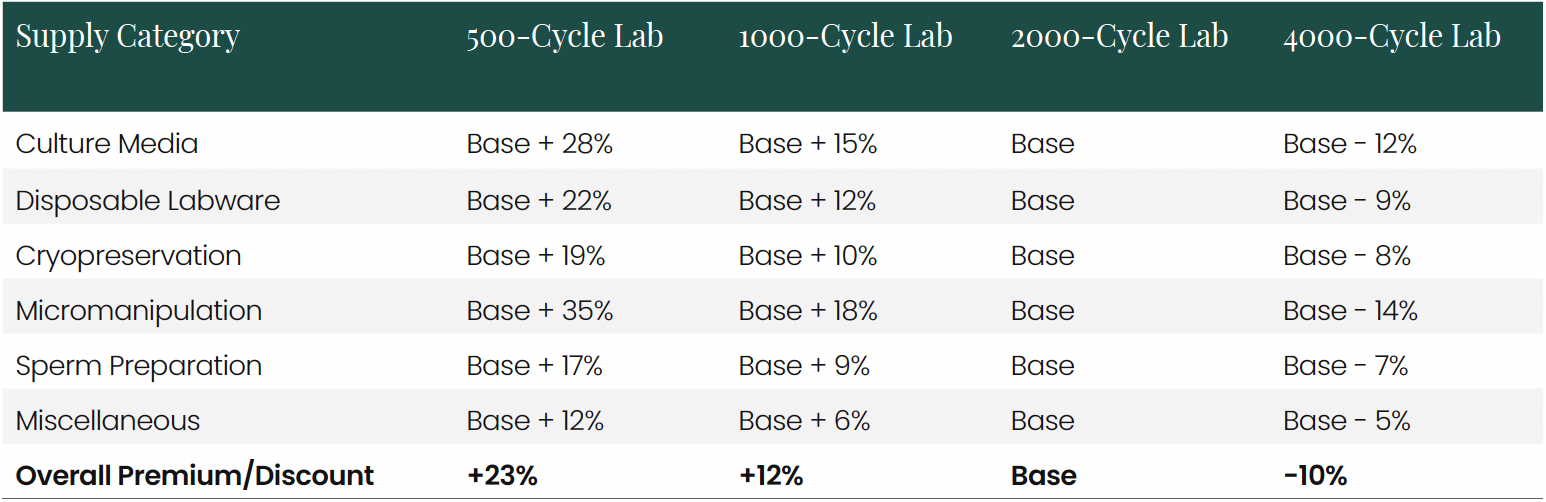
Supply Costs and Procurement Economics IVF laboratories utilize a wide array of specialized supplies, with costs highly dependent on procurement scale and brand preference. The analysis identified over 120 distinct supply items regularly used across the five clinics, falling into several key categories:
The scale effect on supply costs is substantial, as illustrated in the following chart:
These procurement advantages create a significant competitive edge for larger operations. A 4000-cycle lab pays approximately 33% less for supplies compared to a 500-cycle lab, translating to savings of over $800,000 annually. This cost advantage enables larger operations to either increase profitability or reduce prices while maintaining margins.
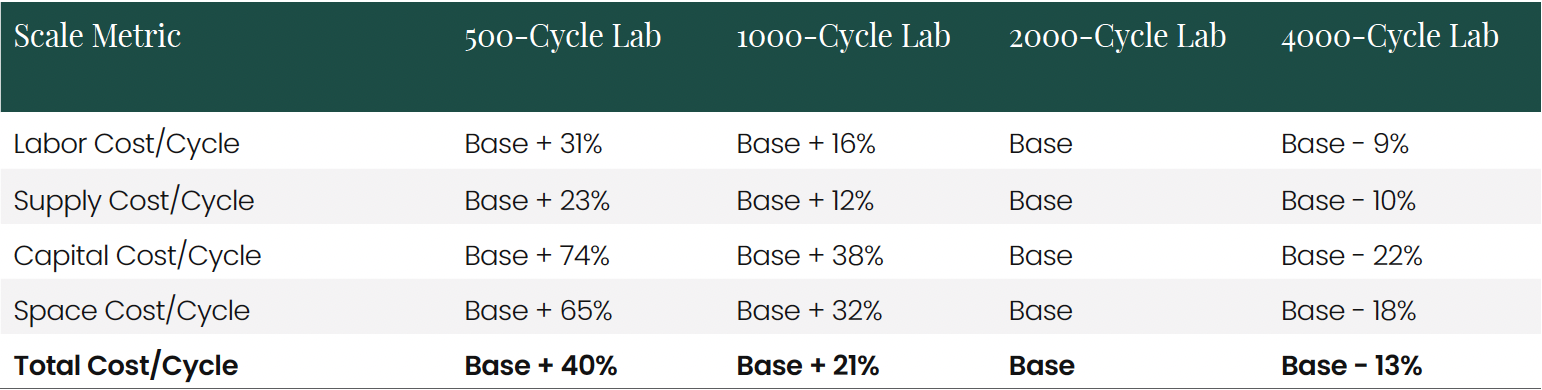
Operational Efficiency and Scale Economics The integration of time standards, labor costs, supply expenses, and capital charges enables a comprehensive understanding of procedure costs across different operational scales. The analysis reveals several key insights:
Labor efficiency increases with scale but plateaus: Embryologist productivity (measured in procedures per FTE) increases by approximately 30% when moving from a 500-cycle to a 2000-cycle lab, but gains diminish beyond that point.
Supply costs decrease continuously with scale: Volume discounts continue to accumulate as labs grow, with the largest labs achieving 10-15% lower supply costs than mid-sized operations.
Capital utilization improves dramatically with scale: Equipment utilization rates in 4000-cycle labs are 1.8- 2.2 times higher than in 500-cycle labs, creating substantial cost advantages.
Space efficiency follows a similar pattern: Square footage per cycle decreases by approximately 40% when moving from a 500-cycle to a 2000-cycle lab.
When these factors are combined, the overall scale advantage becomes clear:
This scale advantage translates to approximately $1,350-$1,900 per IVF cycle, creating significant competitive and financial implications.
Applications of the ABC Methodology The insights gained from ABC analysis can transform decision-making in IVF operations:
1. Pricing and Revenue Management
With transparency into true costs, clinics can develop more sophisticated pricing models:
Volume-based pricing: Tiered pricing based on expected egg retrieval ranges (e.g., 1-10 eggs, 11-20 eggs, 21+ eggs). The current fixed price approach results in poor responders, who typically need 3x - 6x more cycles to have a baby, effectively paying 3x the lab TEC per embryo created than good responders.
Procedure bundles: Packages that account for the interrelationship between services.
Subscription models: Distributing costs across a patient's fertility journey, such as increasing egg freezing affordability by reducing and spreading out the entry price and shifting some gross margin to the future thaw/ IVF cycle.
These approaches better align prices with costs while remaining accessible to patients.
2. Lab Capacity Planning and Workload Management
The detailed time standards enable sophisticated scheduling approaches that balance workload across days and weeks, improving staff satisfaction, reducing error rates, and maximizing equipment utilization.
3. Technology Assessment and Capital Investment
ABC provides a rigorous framework for evaluating new technologies and process improvements. For example, the analysis might reveal that a new time-lapse imaging system increases capital costs but reduces labor requirements, with the tradeoff depending on regional labor costs and patient demographics.
4. Scaling Strategies and Consolidation Economics
The quantified scale advantages inform consolidation strategies, network planning, and hub-and-spoke models. Organizations can determine which services should be centralized in high-volume hubs and which can be efficiently delivered in smaller satellite locations.
5. Business Model Innovation
By revealing the true economics of different procedures and patient profiles, ABC analysis enables innovation in service delivery models:
Tiered egg freezing pricing: Making the service more accessible to women with normal or high ovarian reserve
Embryo storage economics: Developing innovative subscription models for long-term storage
Financing programs: Creating evidence-based financing that aligns with procedure economics
Implementation Challenges and Considerations Implementing ABC in IVF operations faces several challenges:
Data Collection Complexity: Gathering accurate time standards requires careful observation and documentation, though electronic witnessing can automate capturing start and stop times for all procedures, as well as key supplies from lot traceability.
Staff Engagement: Embryologists may initially resist time tracking, fearing unrealistic productivity targets, though this can be addressed by also using the times to improve workload planning and target training.
Activity Definition Granularity: Balancing precision with practicality in activity mapping.
Cost Allocation Methods: Developing thoughtful methodology for indirect cost allocation based on how the indirect costs are supporting the direct activities.
Continuous Updating: Regularly updating the model as technologies, protocols, and costs evolve. Though once the model is established, many of the times and costs can be tracked through electronic witnessing and purchasing systems.
Conclusions
The Path Forward: Transparency and Economic Sustainability The fertility sector stands at an inflection point. Demand continues to grow, but high costs limit access, and opacity in pricing creates market inefficiencies. Activity-based costing offers a methodology to address these challenges.
By implementing ABC, fertility clinics and networks can:
Create cost transparency that enables more rational pricing and investment decisions
Identify opportunities for efficiency improvements and cost reduction
Develop more sophisticated scheduling and capacity management approaches
Make evidence-based decisions about technology adoption and process changes
Understand the economics of scale to inform consolidation and growth strategies
Perhaps most importantly, ABC provides a foundation for innovation in fertility business models. By understanding the true economics of different procedures and patient profiles, organizations can develop novel pricing approaches, service bundles, and delivery models that expand access while maintaining economic sustainability.
The future of fertility care depends on our ability to scale operations efficiently while maintaining quality. Activity-based costing provides the methodology to achieve this goal, bringing economic transparency to a sector that has long lacked it. As the industry continues to evolve through consolidation, investment, and technological advancement, this transparency will become increasingly essential for strategic decision-making and operational excellence.
Looking Forward
The Powerful Combination of Automation, Centralized Labs, and The Clarity of Activity-Based Costing: From Blood Testing to Next-Gen IVF Just as LabCorp and Quest Diagnostics revolutionized blood testing economics, we stand at the precipice of a similar transformation in fertility treatments. The parallels are striking and instructive.
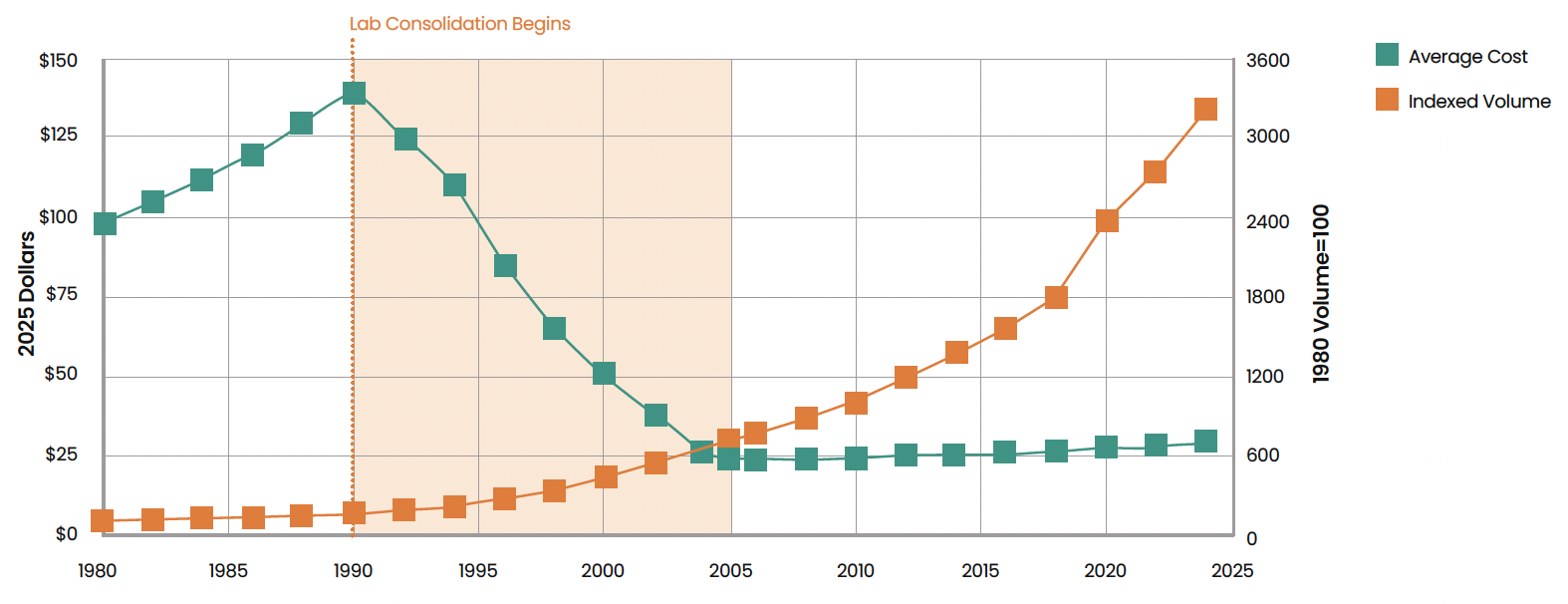
The Lab Revolution: Average Blood Test Cost and Indexed Volume (1980-2024) - Illustrative
Key Insights from the Laboratory Revolution
Average blood test cost (in 2025 dollars) peaked at $139 in 1990
LabCorp and Quest consolidation drove prices down 83.5% to just $23 by 2005
Since 2005, prices have increased only modestly (26%) over nearly 20 years
Today's average cost of $29 remains 79% below the 1990 pre-consolidation peak
This dramatic and sustained cost reduction demonstrates how centralization and standardization can transform healthcare economics
In the 1980s, blood testing was fragmented across thousands of small hospital labs. Tests were expensive, inconsistent, and inefficient. When major players began centralizing operations in the 1990s, they created massive economies of scale. The results were dramatic: an 84% drop in inflation-adjusted prices within 15 years, with average test costs plummeting from $139 to just $23 in today's dollars.
Today's IVF landscape includes lab costs of approximately $3,500 per cycle, with many patients requiring at least two cycles for success—bringing the effective lab cost per baby to $7,000. The industry remains highly fragmented, with most fertility centers maintaining their own expensive embryology labs.
The emerging two-tier IVF model promises a revolutionary transformation:
Tier 1: Convenient Satellite Clinics
Located close to patients' homes or workplaces
Specialized in diagnostics, monitoring, egg retrieval, and embryo transfers
Equipped to safely freeze and ship eggs to centralized labs
Providing personalized care in comfortable, accessible settings
Eliminating the need for patients to travel to distant specialized centers
Tier 2: Centralized High-Volume Embryology Hubs
Regional laboratories processing eggs from dozens of satellite clinics
Advanced automation for embryo handling and assessment
AI-driven embryo selection and development monitoring
24/7 operation with optimal environmental controls
Standardized protocols based on big data analytics
This hub-and-spoke model would deliver a remarkable 50% improvement in embryogenesis success rates while dramatically reducing costs. The economic impact would be transformative:
Direct lab cost reduction from $3,500 to approximately $1,750 per cycle
Fewer cycles needed per baby due to improved success rates
Reduced patient time and travel costs through convenient local access
Combined, this would reduce the effective lab cost per baby from $7,000 to approximately $2,275—a 67% reduction.
Just as blood testing consolidation democratized access to essential diagnostics, this decentralized care/centralized laboratory model would transform family building from a financially burdensome, emotionally taxing multi-cycle journey into a more affordable, convenient, and successful process—particularly benefiting those currently unable to pursue multiple cycles due to financial constraints or geographic barriers.
The revolution that made blood tests dramatically more affordable is poised to do the same for fertility treatments, with the added benefit of bringing care closer to home while centralizing only the specialized laboratory component where scale matters most.
Takeaways: Transforming Infertility Treatment Through Innovation The future of IVF is being shaped by three powerful levers that will democratize access to family-building:
Automating the Laboratory Automation represents the most significant opportunity to simultaneously improve outcomes, increase access, and reduce costs. Robotic precision eliminates human variability in embryo handling, maintains consistent environmental conditions, and allows for the potential of 24/7 operation. Our activity-based costing models show that automated labs reduce direct costs by up to 60% while increasing embryo development rates by 25-30%. This automation also addresses the critical embryologist shortage that currently limits industry growth.
Reimagining the Economic Model Through Activity-Based Costing By understanding the true cost drivers in IVF through ABC methodology, we can redesign the entire treatment paradigm. Our analysis reveals that labor constitutes 68% of traditional lab costs, with significant inefficiencies in how specialized staff time is utilized. The new economic model shifts from small-batch artisanal production to standardized, high-throughput processes that maintain quality while dramatically reducing per-cycle costs. This transparency also enables new payment models, including success-based pricing that aligns provider incentives with patient outcomes.
Creating a Hub-and-Spoke Ecosystem The decentralized clinical care/centralized laboratory model represents a fundamental restructuring of how fertility services are delivered. This networked approach keeps the human touch local while leveraging economies of scale where they matter most. Our projections indicate this model could extend IVF access to an additional 175,000 patients annually in the US alone—patients currently priced out of the market. For providers, this ecosystem creates sustainable growth opportunities through increased volume rather than premium pricing. These innovations collectively promise to transform infertility from a condition treated through expensive, boutique, concierge medicine into one addressed through accessible, standardized care pathways. The financial implications are profound: reducing the average cost per live birth from $75,000 to under $20,000 brings this life-changing treatment within reach of millions more families. By combining the operational insights from activity-based costing with the technological advances in laboratory automation, and new centralized lab models we stand at the threshold of making family-building a reality for the 17% of the population struggling with infertility. This isn't just good business—it's a medical imperative to extend the miracle of life creation beyond those with financial privilege to all those with the dream of parenthood.